The short answer is yes — most of the time. Can you get dental implants with bone loss is one of the most searched questions in implant dentistry for a reason. The verdict often arrives during a single UK consultation, sometimes based on a panoramic X-ray rather than a 3D scan, and feels like a closed door. In most cases, it isn’t.
This guide explains what bone loss actually means for implant candidacy, why a no from a UK dentist isn’t always the final word, and which surgical routes solve dental implants with bone loss cases that other clinics turn away.
Why Jaw Bone Disappears After Tooth Loss?
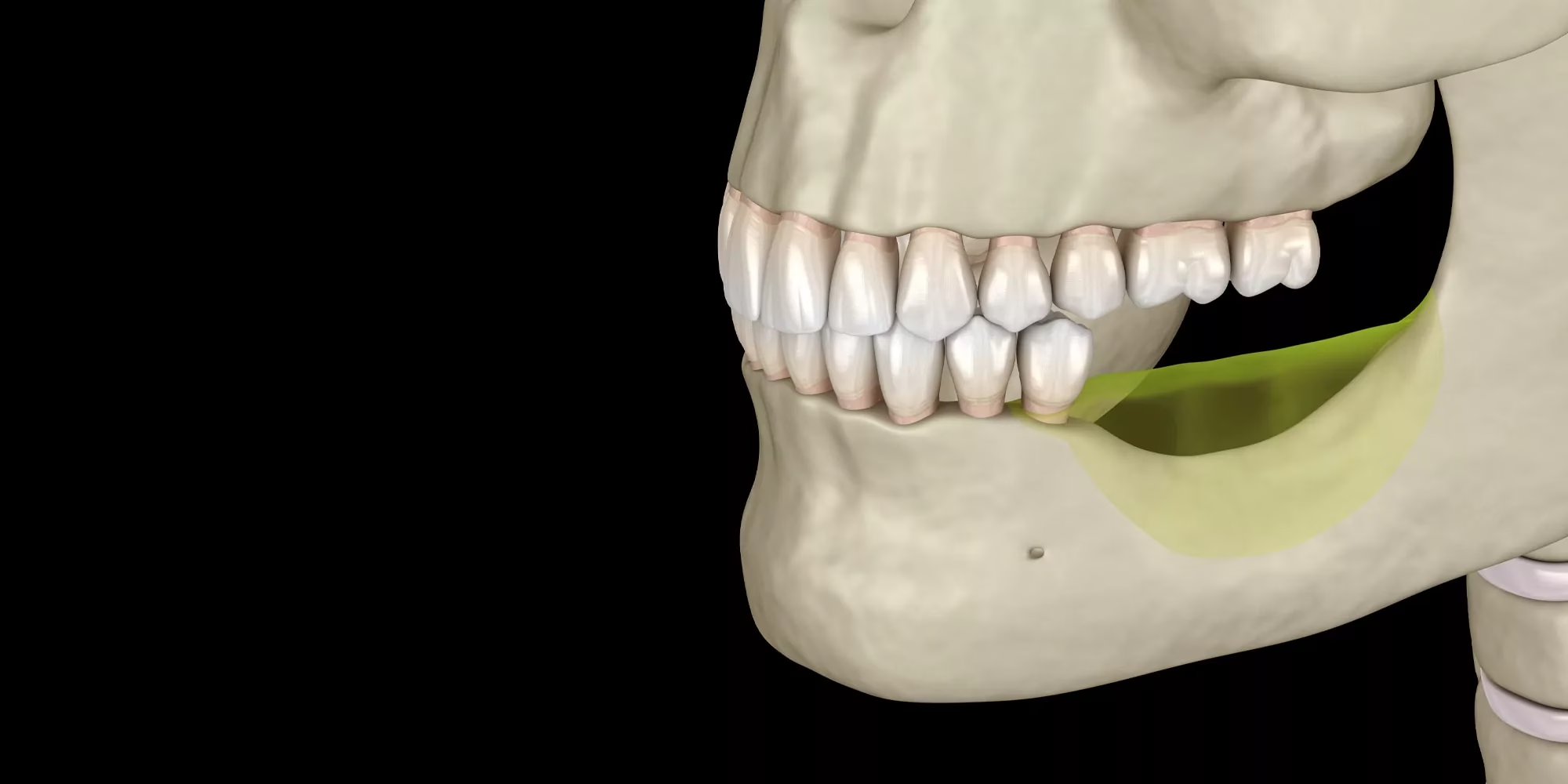
The jawbone behaves differently from the rest of the skeleton. It needs constant stimulation from chewing forces, transmitted through tooth roots, to maintain its volume. When a tooth is removed, that signal stops. Within weeks the body begins reabsorbing the bone around the empty socket, treating it as tissue no longer needed.
The first year after extraction is the worst. Roughly 25% of bone width can be lost in the first twelve months, with continued slower loss for years afterwards. Long-term denture wearers often see additional resorption from the pressure of the plate sitting on unsupported gum tissue. Advanced gum disease accelerates the process further by destroying bone faster than the body can rebuild it.
This is why bone loss is the rule rather than the exception in patients seeking implants. The clinical question is rarely has bone been lost but how much, and what does it mean for treatment.
Book a free consultation with our specialists — we'll build a personalised treatment plan for you.
Can You Have Dental Implants With Bone Loss? It Depends on the Type
The phrase bone loss covers three different measurable problems, and each has its own answer.
Vertical height is the distance between the top of the ridge and a critical structure below — the maxillary sinus in the upper jaw, the inferior alveolar nerve in the lower. Standard implants need around 10mm of usable height. Less than that, and the case becomes more complex but rarely impossible.
Ridge width is the second factor. An implant requires bone all the way around it for long-term stability. A narrow ridge, sometimes described as knife-edge, won’t accommodate a standard fixture without preparation.
Book a free consultation with our specialists — we'll build a personalised treatment plan for you.
Bone density is the most overlooked. Soft, porous bone in the back of the upper jaw integrates implants more slowly and with less predictability than the dense bone found in the lower front jaw. Density isn’t fixed by grafting; it’s managed through implant choice and longer healing windows.
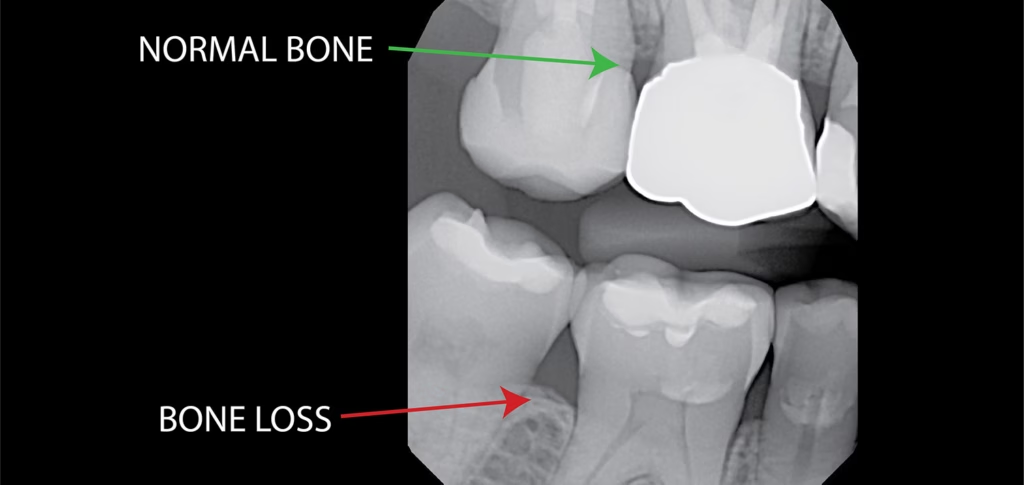
A thorough assessment requires a CBCT scan, which produces a 3D image of the jaw. Two-dimensional X-rays underestimate available bone in a significant proportion of cases. If the assessment that ruled out implants was based only on a panoramic film, the picture may not have been complete.
Mild Bone Loss: Implants Still Go In Normally
Most patients told they have bone loss fall into the mild category, where standard implant placement is still possible with minor adjustments. Shorter implants, available in lengths from 6mm upwards, can be used where vertical height is reduced. Angled placement allows the surgeon to find denser bone in adjacent areas. Modern implant systems are designed for exactly these situations.
Book a free consultation with our specialists — we'll build a personalised treatment plan for you.
Mild dental implants with bone loss cases add little or nothing to treatment time and are considered routine implantology. UK patients in this category are sometimes told they need bone grafting when the case could be managed without it. A second opinion from a specialist who works with shorter and angled fixtures often opens up options that weren’t on the table during the first consultation.
Can You Get Dental Implants If You Have Moderate Bone Loss?
Yes — through bone grafting and sinus lifting, the two procedures that handle the bulk of moderate bone loss cases.
Bone grafting places graft material into the deficient site. The material acts as a scaffold that the patient’s own bone cells migrate into and gradually replace with native tissue over three to six months. The most documented graft material globally is bovine-derived xenograft, used in implant work for over thirty years. Synthetic alternatives are available for patients who prefer them. Once healing is complete, implants are placed into rebuilt bone that behaves like the patient’s original tissue.
Book a free consultation with our specialists — we'll build a personalised treatment plan for you.
Sinus lifting is the upper-jaw equivalent for cases where the maxillary sinus has dropped into the space left by missing back teeth. The sinus floor is gently elevated and graft material packed into the new space below it. Once the graft has matured, implants can be placed into the regenerated bone. This is now considered a routine procedure with predictable outcomes when performed by experienced surgeons.
Treatment with grafting is staged. Surgery is one stage, healing is another, implant placement comes once the new bone has matured, and final crowns follow osseointegration. The total timeline from first surgery to permanent teeth runs nine to twelve months in most cases.
Severe Bone Loss: Implants Without Grafting
Some patients arrive with so much bone gone that grafting isn’t a practical option. Years of denture wear, untreated periodontitis, or congenital conditions can leave a ridge that has too little structure to graft onto. For these cases there are routes that bypass the deficient bone entirely.
Book a free consultation with our specialists — we'll build a personalised treatment plan for you.
Zygomatic implants are longer fixtures anchored into the cheekbone, technically the zygomatic arch, rather than the jaw ridge. The cheekbone is dense, plentiful and unaffected by tooth loss. Two zygomatic implants can support an entire upper arch of fixed teeth, sometimes loaded the same day. This is highly specialist work, performed routinely by only a small number of surgeons internationally. UK access is limited and waiting lists are long. More detail on the technique is available in the zygomatic implant guide.
All-on-4 takes a different approach. Four implants are placed per arch, with the back two angled to take advantage of denser bone in the front of the jaw and avoid the resorbed back regions. One fixed bridge is supported by all four fixtures, often delivered same day. It has become the standard solution for moderate-to-severe full-arch cases where zygomatic placement is more than required but standard implants won’t work. The full procedure is covered in the All-on-4 guide.
These options exist because severe dental implants with bone loss cases have been a solved problem in implantology for over a decade. The reason patients don’t always hear about them is access and clinical familiarity, not science.
Book a free consultation with our specialists — we'll build a personalised treatment plan for you.
Can You Get Teeth Implants With Bone Loss After a UK No?
Three things make the difference between not possible and possible with planning.
The first is a CBCT scan. If the assessment that declined implants was based only on a panoramic X-ray, the picture is incomplete. A 3D scan often reveals more usable bone than a 2D image suggests, and it’s the only image that allows accurate surgical planning.
The second is asking what techniques the original clinic offered. Many general dental practices don’t perform grafting, sinus lifting, or zygomatic placement. A no from a generalist often means not by us rather than not possible. A specialist-led second opinion frequently changes the outcome.
Book a free consultation with our specialists — we'll build a personalised treatment plan for you.
The third is being realistic about timeline. Bone loss cases that involve grafting take nine to twelve months from first surgery to permanent teeth. Cases that go directly to zygomatic or All-on-4 placement can be completed in a single surgical visit. The route depends on the bone, the patient’s preferences, and the surgeon’s recommendation, but very few cases close the door entirely.
For UK patients exploring options abroad, bone loss treatment in Turkey covers the full clinical pathway from CBCT assessment through to permanent prosthesis.